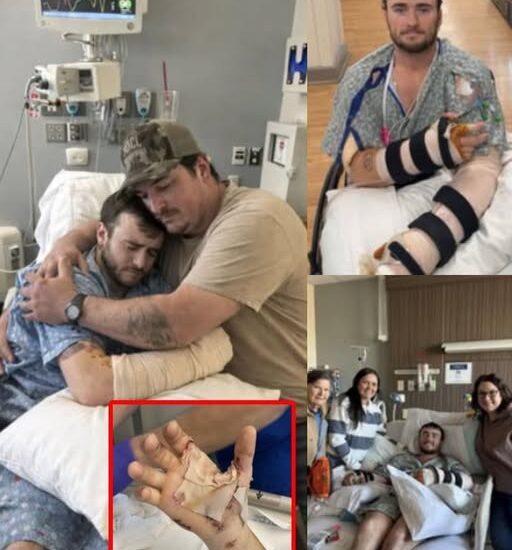
Monitors were steady. Surgeons were cautiously satisfied. Family members finally allowed themselves a fragile breath. After days defined by uncertainty, survival itself carried weight.
⚡ BREAKING: “Goodnight Y’all.” Three Words — And the Room Felt It. ⚡
He made it through another surgery.
For a few hours, that alone felt like victory.
Monitors were steady. Surgeons were cautiously satisfied. Family members finally allowed themselves a fragile breath. After days defined by uncertainty, survival itself carried weight.
But as the sun dipped and hospital corridors quieted, reality returned.
The pain came roaring back.
Especially in his left arm.
And in trauma recovery, pain isn’t just discomfort — it’s information.
When Night Makes Everything Louder
During the day, hospital rooms carry motion. Nurses cycle in and out. Specialists review charts. Conversations create rhythm. There’s momentum.
At night, that momentum fades.
The hum of machines becomes sharper.
The beeps more noticeable.
The body more aware of every sensation.
For Hunter, the left arm pain intensified as evening settled in — deep, relentless, unignorable.
Doctors explain that this kind of pain after complex trauma and surgery can stem from multiple sources: swelling, nerve irritation, tissue inflammation, or circulation fluctuations. Each factor requires close monitoring, especially in the first 24 to 48 hours post-operation.
The wound vacuum — a negative-pressure system designed to promote healing and reduce infection risk — continues to do its job. It draws fluid away from the surgical site, encouraging blood flow and tissue recovery.
But healing is not gentle.
It is active.
And it can be loud.
Why the Left Arm Pain Matters
Pain following surgery isn’t unexpected. However, in cases involving vascular repair or trauma reconstruction, specific pain patterns can signal whether circulation remains strong or if swelling is creating pressure.
That’s why overnight monitoring is critical.
Nurses are checking:
• Capillary refill time
• Skin temperature and coloration
• Pulse strength
• Swelling progression
• Compartment pressure indicators
Circulation is everything in trauma recovery.
If blood flow remains stable, pain may reflect normal inflammatory response. If circulation falters, intervention must be swift.
So far, doctors report that while the pain is significant, vital indicators remain stable.
That distinction matters.
“Goodnight Y’all.”
After hours of discomfort and repositioning, after medication adjustments and quiet reassurances, Hunter said three simple words:
“Goodnight y’all.”
No drama.
No fear in his voice.
Just exhaustion.
For supporters following every update, those words carried more weight than any medical chart.
They signaled something subtle but powerful: resolve.
Closing your eyes after trauma surgery requires trust — trust in the medical team, trust in your body, trust that you’ll wake up stronger than you were before.
It’s a different kind of courage.
And everyone in that room felt it.
Cleared to Leave ICU
Perhaps the most significant development of the day: Hunter has been medically cleared to transfer out of the Intensive Care Unit once a bed becomes available.
That doesn’t mean the fight is over.
But it means the immediate life-threatening phase has stabilized enough to step down a level of care.
ICU discharge signals:
• Sustained stable vitals
• Controlled bleeding
• Managed airway and oxygen levels
• Reduced risk of sudden deterioration
In trauma medicine, movement out of ICU is not symbolic.
It’s earned.
Each stable hour builds toward it.
And Hunter earned it.
Independence, Even Now
Amid pain and exhaustion, there’s another detail that speaks volumes about his mindset.
He’s figuring out how to rig his phone with Velcro so he can use it more easily.
That may sound small.
It isn’t.
Adaptation during recovery reflects resilience. Problem-solving in the middle of discomfort signals mental strength. Independence, even partial, restores dignity in environments where patients often feel powerless.
He isn’t waiting passively.
He’s adjusting.
Engineering solutions.
Refusing to surrender control over the little things.
In long recoveries, those little things matter more than most realize.
What Doctors Are Watching Overnight
As Hunter rests, the medical team remains vigilant.
Overnight priorities include:
• Monitoring for swelling spikes
• Ensuring consistent blood flow
• Tracking pain response to medication
• Watching for early signs of infection
• Evaluating neurological responsiveness
The next 12 to 24 hours will help determine how his body is responding to surgical stress.
If inflammation remains controlled and circulation holds steady, momentum builds.
If complications arise, rapid intervention follows.
That’s the reality of trauma recovery.
Progress is measured hour by hour.
Pain Is Loud. But So Is Strength.
There’s a misconception that recovery gets easier after surgery.
Often, it gets harder before it improves.
Pain intensifies as anesthesia fades. The body begins inflammatory repair. Muscles stiffen. Nerves react.
But pain, when monitored and managed, can be part of forward motion.
Tonight, the machines hum.
The wound vac continues its steady pull.
The ICU staff keeps watch.
And Hunter sleeps — not because the fight is finished, but because rest is part of fighting.
The Bigger Picture
This moment isn’t about dramatic breakthroughs.
It’s about endurance.
It’s about a patient who survived another surgery.
About a left arm that still hurts — but still shows circulation.
About clearance to leave ICU.
About adapting with Velcro and grit.
About three quiet words that told everyone he hasn’t lost his spirit.
“Goodnight y’all.”
Simple.
Steady.
Strong.
📌 What doctors are monitoring most closely overnight, why left arm pain remains a key focus, and what the transfer out of ICU truly signals for his long-term recovery — the full story is in the comments below.



Leave a Reply