🚨 Latest Update on Hunter: A Quiet Moment Inside the NLMC ER Signals Measured Progress
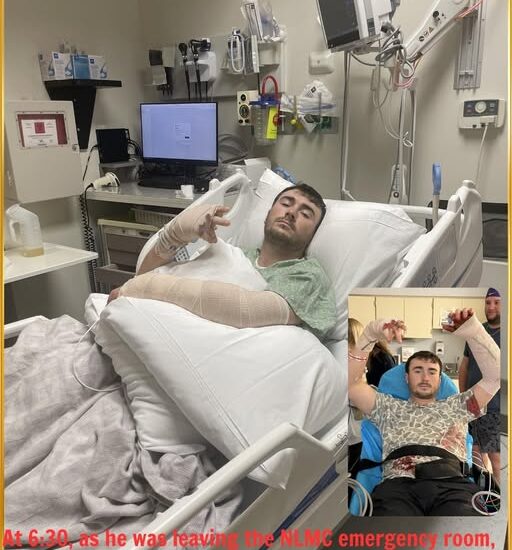
Around 6:30 p.m., just as preparations were underway to leave the emergency room at Northern Louisiana Medical Center, Hunter made a request that caught everyone off guard.
He asked his mom to take a quick photo.
After hours inside the ER — surrounded by monitors, routine vital checks, and hushed but focused exchanges between medical staff — it wasn’t a dramatic moment. It wasn’t urgent. It wasn’t procedural.
It was human.
In a day defined by uncertainty, that small pause felt significant. Not because it changed the medical plan. Not because it signaled discharge. But because it reflected awareness — a desire to hold onto a moment of calm before the next transition.
Within minutes, an ambulance was scheduled to arrive to continue his transport and extended care. The transfer marked another step in a day that had already required extraordinary resilience from both Hunter and his family.
But here’s what shifted the atmosphere inside the room:
His blood pressure returned to normal.
For physicians, that number carries weight. Blood pressure isn’t just a statistic on a screen — it’s a foundational indicator of systemic stability. When it fluctuates, it can signal stress, pain response, dehydration, or more serious underlying complications. When it returns to a normal range after hours of monitoring, it suggests the body is responding to treatment.
It was the first measurable reassurance of the afternoon.
Why That Number Matters
Emergency medicine often operates in layers. Stabilize first. Evaluate second. Plan next steps third.
During Hunter’s time inside the ER, attention centered on maintaining steady vitals and ensuring no additional complications emerged. The medical team closely observed trends rather than isolated readings. A single good number means less than sustained improvement over time.
When his blood pressure normalized and held, it gave doctors something tangible to work with — a baseline from which to proceed more confidently.
It didn’t erase the fragility of his condition.
It didn’t eliminate risk.
But it provided footing.
A Transition, Not a Conclusion
The scheduled ambulance transfer underscores an important reality: stabilization in the ER does not mean resolution. It means readiness for the next phase.
Transport decisions are rarely made casually. They require coordination between facilities, confirmation of bed availability, secure medical documentation, and transport teams equipped for potential changes en route. Every detail matters.
Hunter remains under close watch. Monitoring continues. Evaluations are ongoing.
Doctors are proceeding cautiously not because of new alarms — but because cautious medicine saves lives.
Stability is encouraging. Overconfidence is dangerous. The balance between the two defines high-level care.
The Power of a Pause
The photo Hunter asked for wasn’t about the hospital equipment or the clinical environment. Family members say it was simply about marking the moment.
A breath between storms.
In emergency settings, time blurs. Minutes stretch. Updates feel scarce. The emotional toll compounds quietly. A single intentional act — like taking a photo — can ground everyone involved.
It was proof that amid IV lines and medical charts, there was still space for presence.
Still space for connection.
The Emotional Weight Behind the Scenes
Family members describe the afternoon as tense but steady. Not chaotic — focused. Nurses moved efficiently. Doctors communicated clearly. Questions were answered directly.
The most difficult part, they say, was the waiting.
Waiting for labs.
Waiting for readings.
Waiting for reassurance.
Support messages from friends, extended family, and even distant well-wishers became a quiet source of strength. Prayers and encouragement, though intangible, provided emotional scaffolding in a moment where control felt limited.
Those outside hospital walls often underestimate the endurance required in emergency scenarios. It’s not just the patient who must remain strong — it’s the circle around them.
Tonight, that circle is holding onto one key phrase:
Stability is progress.
Why Doctors Are Still Careful
Even with normalized blood pressure, Hunter remains fragile. Emergency teams know that initial improvement must be supported by continued observation. Secondary complications can develop. Underlying causes require confirmation. Treatment plans evolve based on new information.
That’s why transport is proceeding methodically.
That’s why new evaluations are scheduled.
That’s why optimism remains measured.
Medical caution should not be mistaken for hidden danger — it’s simply best practice.
What Comes Next
As transport continues and new assessments begin, attention will shift from immediate stabilization to broader diagnostic clarity. Additional imaging, specialist consultations, and coordinated care planning are expected components of the next stage.
Each step will build on the stability achieved inside the ER.
Each data point will inform the larger picture.
And through it all, Hunter’s family remains present — steady, hopeful, and realistic.
A Moment That Matters
It’s easy to focus on dramatic updates. Emergency sirens. Urgent interventions. Critical alerts.
But sometimes the most important development is quieter.
A normal blood pressure reading.
A carefully planned transfer.
A son asking his mom for a photo before the next chapter begins.
That moment inside Northern Louisiana Medical Center didn’t mark the end of the journey. It marked a shift.
From crisis to cautious progress.
From uncertainty to measurable stability.
And for tonight, that is enough.
Further details about what occurred in the minutes after that photo — and why physicians are maintaining heightened monitoring despite encouraging signs — are being shared by the family in a follow-up update.
For now, one truth stands:
In emergency care, stability isn’t small.
It’s everything.



Leave a Reply