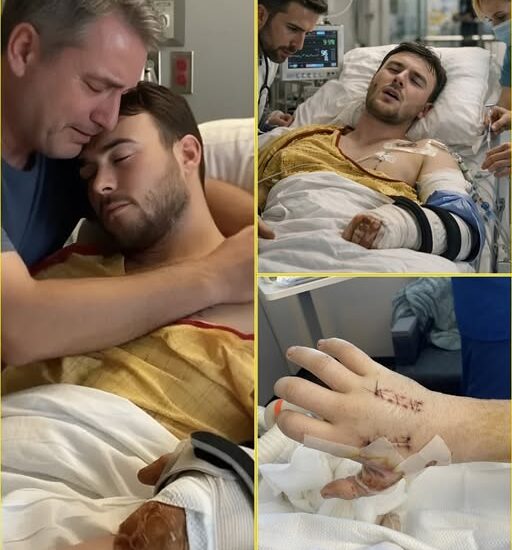
Latest Update on Hunter: Doctors Confront Rapidly Spreading Deep Tissue Infection
🚨 Latest Update on Hunter: Doctors Confront Rapidly Spreading Deep Tissue Infection
Hunter’s recovery has entered another critical phase.
After weeks of surgeries, stabilization efforts, and meticulous wound management, specialists have identified signs of a rapidly spreading deep tissue infection — a complication that can escalate quickly in complex electrical trauma cases if not aggressively contained.
Inside Northern Louisiana Medical Center, the tone has shifted once again.
Focused.
Urgent.
Coordinated.
The Warning Signs Doctors Couldn’t Ignore
Medical teams began noticing subtle but concerning changes during routine monitoring.
Lab markers showed rising inflammatory levels.
Imaging scans revealed suspicious activity beneath the surface — areas where tissue appeared compromised beyond what was previously documented.
Deep tissue infections differ significantly from surface-level wound infections. They can spread along muscle planes and connective tissue layers, sometimes without dramatic external symptoms in the early stages.
That’s what makes them dangerous.
In trauma patients — especially those recovering from electrical injuries — damaged tissue can create an environment where bacteria multiply rapidly. If unchecked, the infection can move into surrounding structures and, in severe cases, enter the bloodstream.
Early detection dramatically improves outcomes.
But timing is everything.
Immediate Escalation of Treatment
As soon as the warning signs emerged, doctors intensified therapy.
Broad-spectrum intravenous antibiotics were initiated immediately to target a wide range of potential bacteria. Infectious disease specialists were brought into the care plan. Additional imaging was ordered to map the full extent of the suspected spread.
Surgical teams are now reassessing tissue viability in real time.
Hunter is under round-the-clock observation. Vitals are being tracked hour by hour. Blood work is being repeated at short intervals to detect shifts in infection markers.
This stage of care is relentless.
There is no passive waiting.
Why Deep Infections Are Especially Concerning
Deep tissue infections in trauma patients present unique challenges:
• Damaged blood vessels may limit antibiotic delivery to affected areas
• Swelling can restrict circulation further
• Necrotic (dead) tissue can harbor bacterial growth
• Symptoms may initially appear subtle
In electrical injuries, internal tissue damage may extend farther than surface wounds suggest. That hidden vulnerability can create pockets where infection thrives.
If antibiotics penetrate effectively and inflammation stabilizes, the infection can often be controlled without immediate surgery.
If not, surgical debridement — the removal of infected tissue — may become necessary.
That decision can unfold quickly.
What Doctors Are Monitoring Now
Over the next several hours, medical teams are closely watching for specific indicators:
• Stabilization or reduction in inflammatory lab markers
• No further expansion on follow-up imaging
• Stable heart rate and blood pressure
• Absence of fever spikes
• Adequate oxygen delivery to affected tissue
Doctors are particularly alert for signs of systemic inflammatory response — a condition in which infection triggers widespread effects throughout the body.
The key threshold they are monitoring involves a combination of lab trends and clinical presentation. If inflammatory markers continue rising despite antibiotics, or if vital signs show instability, emergency surgical intervention may be required sooner than planned.
Every hour matters.
A Shift in the Hospital Atmosphere
Family members describe the mood as serious but steady.
They understand the gravity of a deep infection. But they are holding onto one critical fact: it was caught early.
Specialists emphasize that vigilance is their strongest weapon right now.
No symptom is being dismissed.
No delay is being risked.
Multidisciplinary teams — surgery, infectious disease, critical care — are coordinating continuously. Decisions are being made collaboratively and rapidly.
This is not reactive medicine.
It is proactive containment.
The Compressed Timeline
Infections of this nature tend to declare themselves quickly.
Within 12 to 24 hours, patterns begin to emerge:
Is inflammation stabilizing?
Are antibiotics penetrating effectively?
Is circulation strong enough to support healing?
Or is infected tissue continuing to deteriorate?
Deep infections in trauma patients can either stabilize under aggressive therapy — or force urgent surgical decisions designed to prevent systemic spread.
That is the crossroads Hunter’s team is approaching.
Why Early Detection Changes the Equation
The fact that specialists identified the infection before overt systemic collapse is significant.
Early-stage containment dramatically improves survival rates and functional outcomes. By initiating antibiotics at the first credible sign of spread, doctors have positioned themselves ahead of the curve.
But caution remains essential.
In trauma recovery, stability can shift quickly.
The Next Critical Hours
Tonight, antibiotics are running continuously.
Scans are being reviewed repeatedly.
Nurses are documenting even the smallest change in temperature, pulse, or wound appearance.
Surgeons remain on alert.
If the infection responds — if lab values plateau or decline — the current course may hold.
If it accelerates, operating room preparations could move from standby to immediate action.
This is the delicate balance of complex trauma care: aggressive vigilance without premature intervention.
Is This Contained — or Escalating?
That question cannot yet be answered definitively.
But one thing is clear: the medical team is moving fast, and they are not underestimating the threat.
Hunter remains under intense observation. His fight has already required resilience beyond measure. Now, precision and timing will determine the next chapter.
Is this a contained complication — or the most dangerous turn in his recovery so far?
What doctors are watching for overnight — and the specific threshold that could trigger emergency surgery — is detailed in the comments below. 👇



Leave a Reply