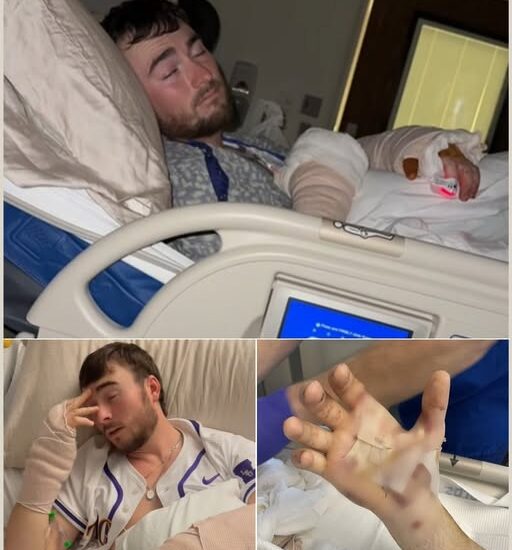
Latest Update on Hunter: ICU Monitoring Escalates to Critical Vigilance
🚨 Latest Update on Hunter: ICU Monitoring Escalates to Critical Vigilance
Tonight, the tone inside Hunter’s ICU room has changed.
What began as cautious monitoring has shifted into something far more intense: minute-by-minute scrutiny. Physicians are no longer offering broad reassurances or long-range projections. They are focused on numbers — circulation readings, perfusion markers, lab values — watching each fluctuation in real time.
Hunter’s condition is now being described as critical.
That designation is not dramatic language. In complex post-surgical electrical trauma cases, it reflects a narrow physiological margin where even small changes can rapidly cascade.
From Observation to Decision Point
Over the past several days, Hunter has been recovering from severe electrical trauma and multiple surgeries aimed at preserving viable tissue and stabilizing systemic function. Early stabilization phases required careful fluid balancing, infection prevention, and protection of surgically rebuilt areas.
Now, the equation has shifted.
Instead of simply maintaining progress, the ICU team is guarding against potential deterioration.
Machines hum steadily at his bedside:
-
Oxygen saturation monitors
-
Arterial blood pressure lines
-
Continuous vascular flow tracking
-
Neurological response assessments
Specialists rotate in quietly — trauma surgeons, critical care physicians, vascular experts — reassessing data as it updates.
No one is stepping far from the room.
In electrical trauma recovery, complications can develop quickly and without dramatic warning. A subtle lab shift at 9:00 p.m. can become a surgical emergency by midnight if not caught early.
The team knows this.
That’s why tonight is different.
The Threshold Doctors Identified
Earlier today, physicians flagged a specific threshold tied to tissue perfusion and systemic stability.
Perfusion refers to the delivery of oxygenated blood to tissues. After electrical injury and surgical reconstruction, maintaining adequate perfusion is essential. Fragile tissue — especially areas already compromised by voltage damage — depends on steady circulation.
Doctors are watching one particular marker closely:
A measurable indicator of how effectively blood is reaching peripheral tissues and clearing metabolic byproducts.
Hunter is approaching that line.
That does not mean it has been crossed.
It means the margin is thin.
And in trauma medicine, thin margins demand heightened vigilance.
Why Perfusion Is So Critical
Electrical injuries differ from surface trauma because damage often travels internally along vascular and muscular pathways.
Even after damaged tissue is surgically removed, surrounding areas may remain vulnerable.
If perfusion decreases:
-
Oxygen delivery drops
-
Cellular stress increases
-
Swelling can worsen
-
Tissue viability may decline
If systemic instability compounds the issue — such as shifts in blood pressure or inflammatory response — recovery can stall rapidly.
That’s why the ICU team is focused less on outward appearance and more on internal metrics.
Tonight, the story is in the numbers.
Critical Doesn’t Mean Chaos
Despite the gravity of the moment, there is no panic in the unit.
The atmosphere is intense, not frantic.
Nurses check lines and pressures with precision. Physicians review digital trends and compare hour-over-hour lab data. Communication is calm and direct.
This is what critical vigilance looks like:
-
Frequent reassessment
-
Rapid response readiness
-
Proactive intervention planning
Emergency surgical teams have been placed on alert — not because action is certain, but because readiness reduces delay if intervention becomes necessary.
Preparedness is protection.
What Could Happen Next
The next few hours carry significant weight.
If perfusion indicators stabilize — even modestly — the narrative changes. Stabilization would suggest that current interventions are sufficient and that the body is regaining equilibrium.
If the metric crosses the identified threshold, physicians may need to act quickly.
Potential responses could include:
-
Surgical reassessment of compromised tissue
-
Pressure-relieving procedures
-
Vascular intervention
-
Escalated circulatory support
These decisions are not made lightly. Each additional procedure carries its own risks. But allowing compromised tissue to deteriorate unchecked carries greater danger.
That balance is what doctors are calculating tonight.
The Emotional Reality at the Bedside
Hunter’s family remains present.
They watch the monitors glow in the dim ICU light. They listen to measured updates from staff. They ask careful questions and absorb answers that are technical but transparent.
There is no dramatic outburst.
Only endurance.
In moments like this, families learn to read the tone of the room more than the words spoken. They recognize when physicians shift from general progress updates to precise physiological discussions.
They understand what “critical” means — not hopeless, but fragile.
Why Electrical Trauma Is So Unpredictable
High-voltage injuries create complex recovery paths because damage is often layered:
-
Surface burns
-
Deep muscle injury
-
Vascular compromise
-
Neurological stress
-
Systemic inflammatory response
Even after successful surgeries, the body can react unpredictably. Swelling, microvascular clotting, or inflammatory cascades can alter stability quickly.
That’s why ICU monitoring escalates rather than relaxes in certain phases.
And tonight is one of those phases.
A Narrow Window
The line Hunter is approaching is not a cliff.
It is a warning boundary.
Crossing it does not guarantee emergency — but it significantly increases risk.
Remaining just above it, and trending upward, could mark another narrowly avoided crisis.
That’s the tension in the room.
Not certainty.
Possibility.
What Matters Most Right Now
The medical objective tonight is simple:
Prevent escalation.
Every intervention — medication adjustments, fluid recalibration, oxygen optimization — is aimed at stabilizing perfusion and protecting systemic balance.
If the body responds, this intense period may pass without surgical return.
If not, rapid decisions will follow.
For now, Hunter remains under constant observation.
Machines steady.
Teams alert.
Family present.
The numbers will tell the story.
And in the next few hours, those numbers may determine whether tonight becomes another close call — or the moment that demands immediate action.



Leave a Reply