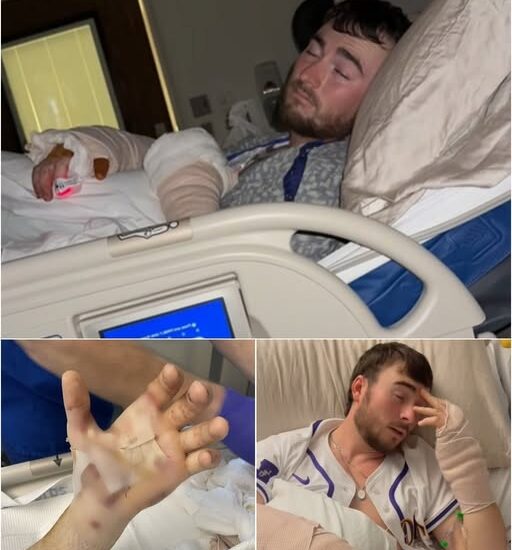
Latest Update on Hunter: The Room Grew Quieter — And the Margin for Error Just Tightened
🚨 Latest Update on Hunter: The Room Grew Quieter — And the Margin for Error Just Tightened
Tonight, the ICU didn’t grow louder.
It grew quieter.
After days of guarded stability, something shifted. Not dramatically. Not with alarms blaring or urgent calls echoing down the hallway. But in numbers. In subtle fluctuations. In readings that refused to settle the way they had before.
Inside the intensive care unit, doctors are no longer speaking in reassurances.
They’re watching monitors — minute by minute, variation by variation.
And what began as careful observation has entered a more decisive phase.
When Stability Starts to Waver
Earlier today, there were signs of strain.
Circulation pressures required adjustment.
Inflammatory markers ticked upward.
Oxygen delivery to vulnerable tissue became less predictable.
None of it catastrophic on its own.
But together, enough to shift the atmosphere in the room.
In complex trauma cases like Hunter’s, it isn’t a single number that alarms physicians. It’s the pattern. The trend. The direction.
And tonight, the trend demanded closer attention.
Why Patterns Matter More Than Moments
In the ICU, isolated readings can mislead. Blood pressure dips briefly. Oxygen saturation fluctuates during repositioning. Swelling changes with fluid shifts.
But sustained variability tells a different story.
Doctors are now focused on three key areas:
1. Perfusion Stability
Blood flow to already compromised tissue must remain consistent. When perfusion becomes intermittent, tissue survival is threatened.
2. Compartment Pressures
Swelling inside muscle compartments can quietly rise again, compressing blood vessels from within. Even slight increases matter when tissue is already stressed.
3. Systemic Inflammatory Response
Elevated inflammatory markers suggest the body is under renewed strain — whether from infection, tissue breakdown, or immune overactivation.
When these indicators begin shifting together, urgency follows.
The Subtle Shift
There was no dramatic collapse.
No code called overhead.
But circulation pressures required recalibration. Medications supporting vascular tone were adjusted. Anti-inflammatory management intensified.
Oxygen delivery — once more predictable — became inconsistent in brief intervals.
For damaged tissue, inconsistency is dangerous.
Cells rely on steady oxygen supply. When delivery fluctuates, they shift into stress mode. Prolonged stress leads to irreversible damage.
That threshold — the one discussed quietly days ago — is about sustained viability.
Not whether tissue survives a single hour.
But whether it can continue surviving under prolonged strain.
Inside the ICU Tonight
Machines hum steadily.
Specialists rotate in with focused efficiency — vascular surgeons, critical care physicians, nursing staff trained to detect even the smallest deviation.
No one lingers in the hallway now.
No one leaves for long.
Hunter remains sedated. His body is fighting. Swelling is being managed aggressively with elevation protocols and medication adjustments. Fluid balance is recalculated repeatedly to avoid worsening compartment pressure.
There has been no irreversible declaration.
But there is unmistakable urgency.
The Narrowing Window
When blood flow becomes inconsistent in already compromised tissue, the window for intervention narrows quickly.
Doctors are watching closely for:
-
Sustained Doppler signals in affected vessels
-
Stable tissue oxygen saturation
-
Controlled compartment pressures
-
Downward-trending inflammatory markers
If perfusion stabilizes, tissue remains viable.
If variability increases, decisions become more aggressive.
The difference can unfold over hours.
What May Have Triggered the Shift?
Physicians are considering several possibilities behind today’s subtle decline:
Delayed Vascular Spasm
Electrical trauma can cause blood vessels to constrict unpredictably days after the initial injury.
Secondary Swelling
Inflammatory cycles sometimes peak later, causing renewed internal pressure.
Infection-Related Stress
Even controlled infections can increase systemic inflammation, affecting microcirculation.
Microvascular Clotting
Small clots in damaged vessels can reduce localized blood flow without immediately obvious signs.
None of these are confirmed publicly.
But each remains under active evaluation.
A Family Holding Its Breath
For Hunter’s family, time feels suspended.
Screens glow in the dim room. Hands clasp tightly. Conversations are whispered.
Every subtle change draws a breath.
Every recalibrated medication brings cautious hope.
There has been no dramatic collapse.
But the margin has tightened.
And when the margin tightens, silence often follows.
Why the Next Hours Matter Most
Doctors are now watching for one thing above all:
Stabilization.
Not improvement.
Not dramatic recovery.
Just consistency.
Consistent blood flow.
Controlled internal pressure.
Predictable oxygen delivery.
If those hold, the path forward remains open.
If they falter, surgical reassessment may come sooner than anticipated.
In cases like this, decisive moments rarely announce themselves loudly. They emerge gradually — in numbers that drift, in readings that hesitate.
Where Things Stand Tonight
Hunter is still fighting.
Circulation is present — but variable.
Inflammation is elevated — but being addressed.
Tissue viability remains — but under stress.
The room is quieter because everyone understands what this phase represents.
It is no longer about whether he survived the initial trauma.
It is about whether his body can maintain equilibrium under sustained pressure.
The next several hours matter more than they have before.
And while there has been no irreversible shift, there is a clear recognition inside the ICU:
The balance is delicate.
Doctors remain vigilant. Adjustments continue. Intervention options remain available.
But tonight, more than any night so far, the outcome depends not on a single breakthrough —
But on whether stability returns.
And stays.



Leave a Reply