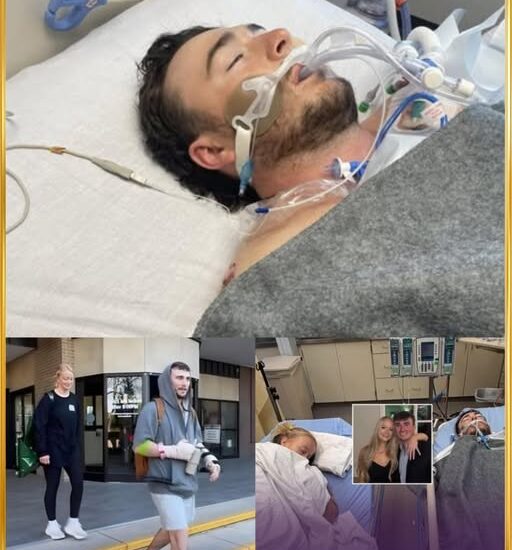
At 12:40 PM, Hunter was rushed back into the operating room after doctors identified rapidly escalating signs of compartment syndrome — one of the most dangerous complications in trauma recovery.
🚨 BREAKING: Emergency Surgery at 12:40 PM — Doctors Feared the Worst.
They didn’t wait.
They couldn’t.
At 12:40 PM, Hunter was rushed back into the operating room after doctors identified rapidly escalating signs of compartment syndrome — one of the most dangerous complications in trauma recovery.
In these cases, pressure builds inside enclosed muscle compartments so quickly that blood flow can shut down entirely. When circulation stops, tissue begins to die. Nerves suffer irreversible damage. Limbs can be lost in hours.
There was no time for debate.
A fasciotomy was the only option.
What Compartment Syndrome Really Means
Compartment syndrome occurs when swelling or bleeding increases pressure within muscle compartments bound by fascia — a tough connective tissue that doesn’t easily stretch.
When pressure rises:
• Blood flow decreases
• Oxygen delivery drops
• Tissue begins to deteriorate
• Nerves lose function
• Pain becomes severe and unrelenting
In advanced cases, untreated pressure can lead to amputation.
For Hunter, the warning signs were unmistakable.
The surgical team moved immediately.
Inside the Operating Room
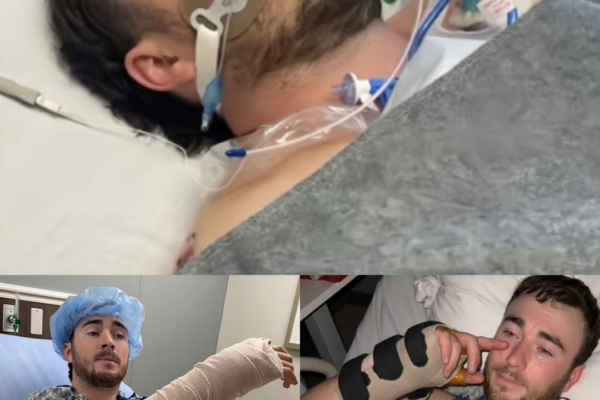
Once in the OR, surgeons made long incisions through the fascia of both arms to relieve pressure and restore circulation.
Only after opening the compartments could they assess the full extent of the damage.
What they found confirmed their fear: compartment syndrome affecting both hands.
Necrotic tissue — tissue that had already begun to die — had to be removed.
The majority of that tissue was located at the base of his thumb. Some muscle was taken from both hands. A small portion was removed from his left forearm.
Every removal was calculated.
Every decision weighed against long-term function.
And then came the line everyone had been holding their breath for:
No amputations were performed today.
Those words shifted the atmosphere instantly.
Relief, cautious but real.
Why the Wounds Were Left Open
After relieving pressure and removing compromised tissue, surgeons did not close the incisions.
That was intentional.
In cases of compartment syndrome, wounds are often left open to prevent renewed pressure buildup. Closing too early can recreate the very conditions surgeons are trying to eliminate.
Instead, wound vacuum systems were placed.
These devices:
• Remove excess fluid
• Reduce swelling
• Improve blood flow
• Lower infection risk
• Promote healing from the inside out
Another surgical debridement — a procedure to remove additional damaged tissue if necessary — is likely within 48 hours.
The full picture will take time.
One day at a time.
One prayer at a time.
Back to the Surgical ICU
At 4:30 PM, Hunter returned to the surgical ICU.
Still intubated.
Still sedated.
But responsive.
He followed commands.
He attempted to speak around the breathing tube.
His vital signs remained stable.
And perhaps most encouraging of all: he is breathing partially on his own. Once he can sustain independent respiration, the medical team will remove the tube.
That step will mark another milestone.
Agitation Is a Sign of Fight
He’s restless.
He wants the breathing tube out.
He wants his hands untied from protective restraints designed to prevent accidental tube removal.
That frustration?
Doctors view it as a positive sign.
Agitation in this context often reflects neurological awareness and cognitive engagement. It means the brain is responding. It means sedation is being metabolized. It means he understands his surroundings.
It means he’s fighting.
What Surgeons Will Be Watching Next
The next 48 hours are critical.
Doctors are closely monitoring:
• Sustained blood flow to both hands
• Skin coloration and warmth
• Capillary refill time
• Swelling progression
• Signs of infection
• Muscle viability
• Nerve responsiveness
Circulation must hold.
Pressure must remain relieved.
Infection must be prevented.
If blood flow remains strong and tissue stabilizes, additional reconstructive planning can begin.
If complications arise, further intervention may be required.
This phase is about stabilization.
The Road Ahead
Doctors are clear: recovery will be long.
Potential next steps may include:
• Additional debridement procedures
• Skin grafts
• Reconstructive surgeries
• Months of intensive physical therapy
• Occupational therapy to preserve function
There are no guarantees regarding long-term dexterity or strength.
But tonight, one fact stands firm:
His hands are still there.
That matters.
Managing Danger, Not Eliminating It
The immediate threat of unchecked compartment syndrome has been addressed.
But trauma recovery doesn’t eliminate danger in a single surgery.
It manages it.
Swelling can fluctuate.
Tissue response can change.
Infection risk remains elevated.
Doctors are not declaring victory.
They are declaring vigilance.
A Community Holding Its Breath
Across social media and within hospital hallways, support continues to pour in.
The emotional weight of today’s surgery was immense.
But so was the relief.
No amputations.
Stable vitals.
Neurological response.
Partial independent breathing.
These are not small milestones.
They are foundations.
Tonight’s Reality
He is sedated.
He is intubated.
He is restrained for safety.
But he is responsive.
He is fighting.
And his circulation — for now — is holding.
What surgeons saw when they opened his arms confirms how close this came to a far different outcome.
What the next 48 hours reveal will determine how well blood flow sustains and whether tissue continues to survive.
The danger hasn’t vanished.
It’s simply being managed.
👉


Leave a Reply