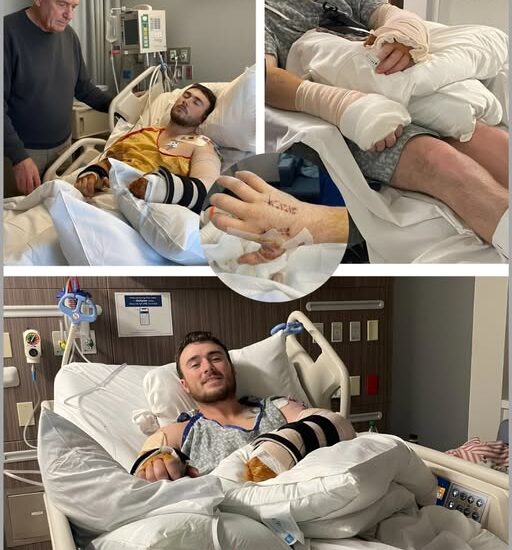
BREAKING — A TURNING POINT NO ONE DARED TO HOPE FOR
🚨 BREAKING — A Turning Point No One Dared to Hope For
4:30 p.m.
After more than four agonizing hours inside the operating room, the doors finally opened. Family members who had been pacing the hallway froze in place.
The lead surgeon stepped forward.
This time — he was smiling.
Then came seven words that instantly reshaped the trajectory of Hunter’s fight:
“We didn’t have to remove any more muscle tissue.”
For weeks, every update had centered on loss — tissue lost, strength lost, stability lost. This time, the message was preservation.
And in a battle against aggressive necrosis, preservation is everything.
🛑 The Spread Has Stopped
Doctors confirmed that the necrotic progression in Hunter’s left arm has halted — at least for now.
That single surgical outcome carries extraordinary weight.
It means:
-
The internal tissue death is no longer advancing.
-
The feared domino effect into surrounding muscle groups did not occur.
-
Blood flow to adjacent areas appears stable enough to sustain viability.
In complex soft-tissue infections or post-traumatic necrotic cases, surgeons often operate with one central goal: stay ahead of the spread. If dead tissue continues expanding, it must be removed to prevent systemic infection.
Today, that escalation did not happen.
After weeks of bracing for further amputation-level discussions, the medical team delivered something different.
Control.
✂️ A Surgical Shift: From Expansion to Closure
In prior procedures, each trip to the OR meant more removal.
Today marked the first time surgeons were able to pivot toward reconstruction rather than reduction.
Instead of widening the incision to chase dying tissue, doctors were able to close a significant portion of the surgical site on Hunter’s left arm.
Closure.
Not expansion.
Not escalation.
Closure.
That shift dramatically improves outlook across several fronts:
💪 Future Mobility
Preserving muscle mass increases the likelihood of regaining functional range of motion during rehabilitation.
🦾 Strength Retention
Each avoided excision protects motor capacity and structural stability.
🔄 Long-Term Recovery Timeline
Moving from debridement (removal) to closure suggests improved tissue viability and infection control.
Medical experts note that in limb-threatening cases, the moment surgeons can stop cutting and begin closing is often the first true sign that the tide is turning.
This is not cosmetic progress.
It is structural victory.
🌊 The Emotional Whiplash of the ICU
For nights, alarms echoed through intensive care corridors. Monitors flashed irregularly. Family members learned to read numbers on screens as if they were a second language.
They prepared themselves for worst-case scenarios.
Repeated surgeries.
Repeated anesthesia.
Repeated uncertainty.
Today’s update did not declare total victory.
But it marked something profoundly different: momentum.
For the first time in weeks, hope did not feel fragile.
It felt grounded.
🔬 What Doctors Are Watching Next
Medical teams are cautious by design. No one is declaring the crisis over. The next 72 hours are critical in determining whether today’s breakthrough holds.
Here are the primary indicators being monitored:
1️⃣ Tissue Perfusion Stability
Doctors will track whether blood flow to the repaired area remains consistent. Poor perfusion could reverse gains quickly.
2️⃣ Infection Markers
White blood cell counts, C-reactive protein (CRP), and other inflammatory markers will reveal whether the infection is truly contained.
3️⃣ Systemic Inflammatory Response
Even localized improvement must translate to overall body stabilization. Persistent systemic inflammation could complicate recovery.
4️⃣ Early Nerve Activity Signals
Preserved muscle only matters if nerve pathways remain viable. Subtle neurological assessments will help determine long-term functional prognosis.
These metrics will guide whether doctors continue with gradual closure and reconstruction — or must intervene again.
⏳ Why the Next 72 Hours Matter
In cases involving aggressive tissue damage, stabilization often proves itself not immediately — but over time.
If:
-
No new necrosis appears,
-
Infection markers trend downward,
-
Vital signs remain steady without escalating support,
Then physicians can cautiously declare the spread halted.
However, if inflammatory signals spike or tissue viability declines, the surgical team may need to reassess strategy.
For now, the trajectory is positive.
But guarded.
💙 The Meaning of Preservation
In severe limb cases, there are moments when expectations quietly lower. Families begin preparing for partial loss. Doctors speak carefully about “functional adaptation.”
Today disrupted that downward narrative.
Instead of discussing how much more might be removed, the conversation turned toward what can now be saved.
Saved muscle.
Saved structure.
Saved possibility.
And that changes everything.
🏥 The Broader Medical Reality
Necrotic progression can be unpredictable. Even with aggressive antibiotics and meticulous debridement, spread sometimes continues despite best efforts.
Halting it requires:
-
Effective antimicrobial coverage
-
Adequate blood supply
-
Surgical precision
-
Patient resilience
Today’s outcome suggests those elements aligned — at least in this critical window.
It is a testament not only to surgical skill, but to Hunter’s physiological fight.
⏭ What Comes After Stabilization?
If the next several days confirm durable stability, doctors may begin discussing:
-
Gradual wound closure completion
-
Physical therapy planning
-
Long-term mobility projections
-
Scar management and reconstructive options
Rehabilitation will not be simple.
Muscle trauma requires months of structured therapy to restore strength and coordination.
But rehab is a forward-looking conversation.
And forward is a direction the family has not felt in weeks.
A Turning Point — Not the Finish Line
Today was not the end of the battle.
But it was the moment the tide shifted.
For weeks, every update carried tension.
Today carried relief.
Seven words from a surgeon changed the emotional temperature of an entire hospital corridor.
“We didn’t have to remove any more muscle tissue.”
In critical care, sometimes survival is measured not by dramatic victories — but by what no longer needs to be taken away.
And tonight, for the first time in a long while, the fight feels less like defense… and more like recovery.

Leave a Reply