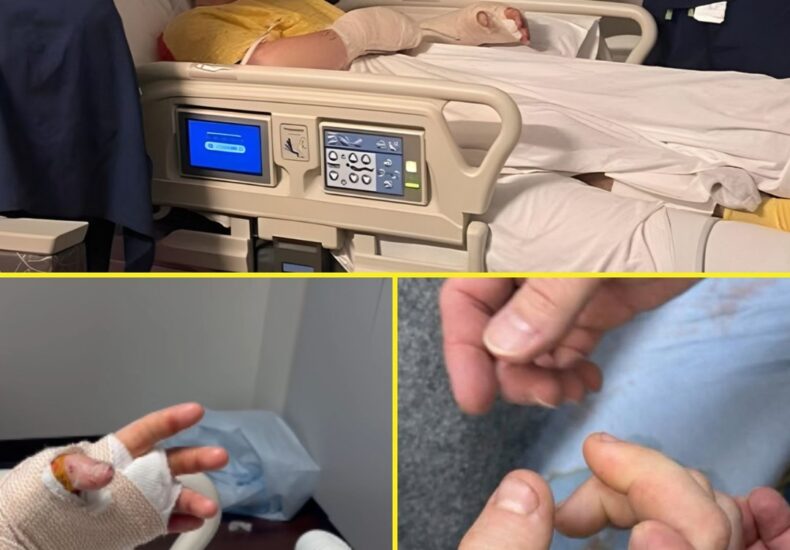
Latest Update on Hunter: Doctors Say Time Is No Longer Measured in Weeks — It’s Measured in Hours
🚨 Latest Update on Hunter: Doctors Say Time Is No Longer Measured in Weeks — It’s Measured in Hours
The tone inside Hunter’s hospital room has changed again.
After days of careful stabilization and round-the-clock monitoring, physicians have delivered a sobering but focused message: recovery is no longer being tracked week by week. It is being measured hour by hour.
According to specialists overseeing his care at Northern Louisiana Medical Center, Hunter may require two to three additional surgical procedures in the coming days. The objective is urgent but precise — preserve as much viable tissue as possible before the window for optimal intervention narrows further.
This phase of treatment is not about dramatic announcements.
It is about timing.
Why Electrical Injuries Are Unpredictable
High-voltage electrical trauma is unlike many other forms of injury. While burns and visible wounds draw immediate attention, the most serious damage often occurs beneath the surface.
Electrical current can travel through muscle, blood vessels, and nerves, generating heat internally. That internal heat may not fully declare itself for days. Tissue that appears stable can deteriorate as swelling increases or circulation becomes compromised.
Doctors explain that evolving tissue injury follows a dangerous pattern:
• Reduced blood flow
• Swelling that restricts oxygen delivery
• Cellular death (necrosis)
• Risk of infection spread
The challenge is identifying the precise moment when damaged tissue crosses from salvageable to unsalvageable.
Act too early, and surgeons may remove tissue that could have recovered.
Wait too long, and infection or systemic complications may spread.
That is the razor’s edge physicians are walking now.
Two to Three More Procedures: What That Means
When doctors discuss multiple back-to-back surgeries in trauma care, it does not necessarily signal failure. In fact, staged procedures are often strategic.
In Hunter’s case, surgeons are evaluating:
• Circulatory integrity
• Tissue viability at surgical margins
• Swelling patterns
• Infection markers
• Functional preservation potential
Each operation would aim to remove only tissue that can no longer survive while protecting nerves, muscle groups, and structural stability wherever possible.
The stakes are high.
Remove too little, and progressive necrosis may continue.
Remove too much, and long-term mobility could be permanently reduced.
Precision now will shape recovery months — even years — from today.
Hour-By-Hour Monitoring
Inside the trauma unit, Hunter’s vitals are being tracked continuously. Specialists are analyzing:
• Blood oxygen levels
• Heart rhythm stability
• Inflammatory markers
• Circulation to affected areas
• Fluid balance and swelling
This phase of care may not look dramatic from the outside. There are no press conferences. No sweeping declarations.
But it is relentless.
Surgical teams review imaging.
Nurses document micro-changes.
Physicians confer repeatedly before any incision is made.
It is a calculated race against progressive tissue damage.
Why the Window Matters
In electrical trauma cases, tissue at risk may enter what doctors call a “gray zone.” It is neither fully alive nor definitively dead.
During this period, the body attempts to restore circulation. If successful, tissue survives. If not, deterioration accelerates.
Surgeons must decide whether to wait for clearer demarcation or intervene preemptively.
That decision is influenced by:
• Temperature changes in affected areas
• Capillary refill times
• Doppler circulation studies
• Worsening laboratory trends
• Signs of systemic infection
The margin for error is narrow.
That is why time is now measured in hours.
Family: Exhausted but Steady
Multiple surgeries within days are emotionally draining — not just physically demanding.
Family members say they understand that repeated procedures are sometimes the only way to stay ahead of progressive damage. Each return to the operating room is not a setback.
It is protection.
An attempt to safeguard future function.
An investment in long-term recovery.
They describe the atmosphere as tense but purposeful. There is urgency, but not panic.
Action, not surrender.
Community Support Inside the Room
Amid the medical intensity, messages of encouragement continue pouring in. Prayers, notes of strength, and quiet words of support have become part of the daily rhythm in the hospital room.
For families navigating complex trauma, community connection can be stabilizing. It reminds them they are not alone in moments when decisions feel overwhelming.
While surgeons focus on precision, loved ones focus on presence.
Both matter.
The Critical Days Ahead
The coming days will likely determine the next chapter of Hunter’s recovery.
If surgeons can successfully preserve viable tissue and prevent infection spread, long-term rehabilitation becomes the focus.
If complications arise, plans may need recalibration.
But doctors emphasize: urgency does not equal hopelessness.
It equals intervention.
It equals proactive strategy.
It equals fighting for every viable centimeter of tissue that can still be saved.
Why Caution Remains Essential
Even with decisive surgical action, electrical trauma remains unpredictable. Swelling patterns may shift. Circulatory flow may improve — or decline.
Physicians are balancing optimism with vigilance.
No assumptions.
No shortcuts.
Every incision carries consequence.
Every delay carries risk.
That is the reality of this stage.
A Defining Moment in Recovery
Hunter remains under close supervision. Specialists are aligning expertise across surgical, vascular, and critical care disciplines to ensure no detail is overlooked.
This is not the dramatic climax of recovery.
It is the disciplined middle — where outcomes are shaped by meticulous judgment.
Time is measured in hours.
Decisions are measured in millimeters.
And hope is measured in preserved function.
Why the tissue remains at risk — and what specific factors doctors are watching before making the first incision — is explained in the comments below. 👇


Leave a Reply