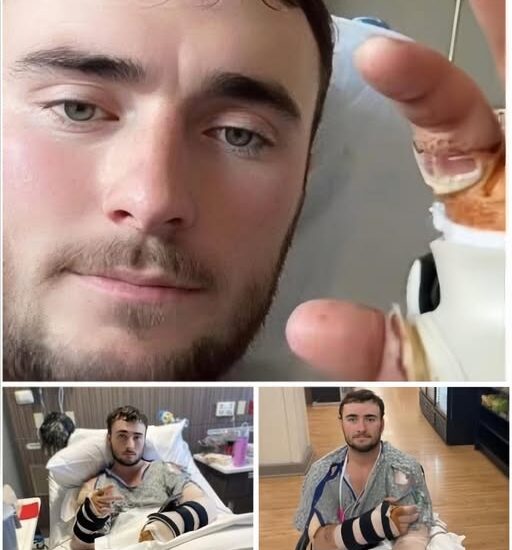
Latest Update on Hunter: Emergency Vascular Surgery After Sudden Circulation Collapse
🚨 Latest Update on Hunter: Emergency Vascular Surgery After Sudden Circulation Collapse
At 8:30 AM CST, Hunter’s recovery took an abrupt and dangerous turn.
After days of cautious monitoring following his high-voltage electrical injury, medical staff detected a sharp decline in blood flow to his arm — a condition doctors described as entering a critical “dead zone,” where circulation becomes too limited to sustain healthy tissue.
Within minutes, he was rushed into emergency vascular surgery.
By 8:45 AM, the operating team was fully engaged.
Their mission is urgent and precise: restore circulation before oxygen deprivation causes irreversible damage. In vascular emergencies, time is not abstract — it is measurable in tissue survival. Muscles and nerves deprived of oxygenated blood can begin deteriorating quickly. The window for preservation can narrow in less than an hour.
This was one of those moments.
Why Circulation Can Suddenly Fail After Electrical Trauma
Hunter’s original injury involved 13,000 volts — an immense electrical force capable of damaging far more than skin.
Electrical trauma often causes deep internal injury to blood vessels, muscles, and nerves. Even when surface wounds appear stable, the vascular system beneath may remain vulnerable. Swelling can increase gradually. Clots can form. Vessels weakened by heat injury may collapse or constrict.
In complex burn cases, vascular compromise can develop suddenly — even after days of apparent progress.
That is precisely what specialists observed this morning: a measurable and dangerous drop in perfusion to the affected limb.
Doctors described it not as chaos — but as a critical turning point.
The “Dead Zone” Explained
In clinical terms, a “dead zone” refers to an area where blood supply has fallen below the threshold required to keep tissue viable. Without sufficient circulation, oxygen levels drop, waste products accumulate, and cells begin to fail.
Early warning signs can include:
-
Cool temperature in the limb
-
Weak or absent pulses
-
Delayed capillary refill
-
Increasing pain or numbness
-
Changes in color
Monitoring teams detected the shift quickly — a crucial factor in what happened next.
Because in vascular emergencies, minutes matter.
Inside the Operating Room: Precision Under Pressure
Hunter remains under anesthesia as surgeons work to reopen pathways, relieve pressure, and reestablish blood flow.
Emergency vascular procedures demand extreme precision. Surgeons must identify the exact cause of compromise:
-
Is a clot obstructing flow?
-
Is swelling compressing a vessel?
-
Has a vessel wall weakened or collapsed?
-
Is compartment pressure rising to dangerous levels?
Each possibility requires a different intervention.
Clots may need removal.
Compressed vessels may require decompression.
Severely damaged arteries may demand bypass grafting or repair.
Once flow is restored, surgeons must also confirm stability. It is not enough to see blood return briefly — circulation must remain consistent and strong before the incision can be closed.
The Key Indicator Surgeons Are Watching
One of the most important signs during vascular repair is the return of bright, pulsatile arterial bleeding — a visible confirmation that oxygenated blood is moving through the repaired pathway.
Surgeons also monitor:
-
Doppler ultrasound signals
-
Tissue color change
-
Temperature normalization
-
Capillary refill speed
If muscle tissue begins responding and perfusion improves, it signals that the limb remains viable.
If response is delayed or limited, additional intervention may be necessary before closure.
This stage is delicate. Decisions must balance urgency with caution.
A Coordinated, Focused Response
Inside the hospital, the tone is described as intense but controlled.
Not frantic.
Not chaotic.
Coordinated.
Every movement calculated. Every instruction deliberate. Teams trained for vascular crises move with efficiency that comes from preparation and repetition.
Doctors emphasized that early detection provided a critical window to intervene before irreversible damage occurred.
Had the drop gone unnoticed for even a short period longer, outcomes could have shifted dramatically.
What This Means for Long-Term Function
For Hunter’s family, waiting outside the operating room carries a different kind of weight than previous procedures.
This is not about wound cleaning or infection control.
This is about preservation of function.
Restoring circulation means protecting muscle strength, nerve signaling, and long-term mobility. If perfusion stabilizes, rehabilitation remains possible. If tissue loss occurs, reconstructive plans may become more complex.
Vascular emergencies alter trajectories quickly.
But early intervention improves odds significantly.
The Next Critical Hours
The next several hours will reveal whether circulation holds steady after repair.
Surgeons will monitor:
-
Arterial pressure
-
Limb temperature
-
Swelling levels
-
Ongoing blood flow stability
If circulation remains strong, it signals that the limb has crossed a major survival threshold.
If instability persists, additional procedures may be required.
Right now, the outcome is still unfolding.
The Fight Is Active
Hunter’s recovery has already required resilience — from careful debridement to infection management and constant reassessment. But vascular compromise introduces a different level of urgency.
It compresses timelines.
It raises stakes.
It forces rapid decision-making under pressure.
Yet there is reason for guarded optimism: the problem was detected early, and surgical teams acted immediately.
That matters.
For now:
The surgical team is working.
The circulation repair is underway.
The outcome is not yet written.
Beyond the operating room doors, his family waits — aware that this chapter may determine long-term function in his arm.
And inside, under surgical light, doctors are doing what they trained for:
Fighting to restore flow.
Fighting to protect tissue.
Fighting for preservation.
Updates will depend on how circulation responds once repairs are complete — and whether the limb shows the signs surgeons are watching for before closing the incision.
The next hours will tell the story.
For now, the effort continues.
You may also like
Calendar
| M | T | W | T | F | S | S |
|---|---|---|---|---|---|---|
| 1 | ||||||
| 2 | 3 | 4 | 5 | 6 | 7 | 8 |
| 9 | 10 | 11 | 12 | 13 | 14 | 15 |
| 16 | 17 | 18 | 19 | 20 | 21 | 22 |
| 23 | 24 | 25 | 26 | 27 | 28 | 29 |
| 30 | 31 | |||||

Leave a Reply